Understanding “Strawberry Skin” aka Keratosis Pilaris
What causes KP — and how do you manage these dry, rough bumps on your skin?
Published:
4 minute read
Ever get those small, rough bumps on the back of your arms, or maybe your thighs? They’re not pimples, and they’re not ingrown hairs…so exactly what are they?
It could be keratosis pilaris — commonly known as chicken skin or sometimes, strawberry skin. While these often dry, bumpy patches aren’t harmful, they can be frustrating to manage. We’re uncovering everything you need to understand about KP: what it is, what causes it, and what you can do to treat it.
Article Quick Links
What is keratosis pilaris?
KP is a buildup of excess keratin (aka hyperkeratinization) inside the pores that results in a hardened plug of protein — that characteristic rough bump. Remember that keratin is the most abundant protein in your hair, skin and nails, and is made up of various amino acids. It provides the protective structure, or scaffolding, of the epidermis.
Here’s where things get fuzzy, because exactly what sets off this abnormal keratinization in the first place is still very much up for debate. There are a few theories being investigated, including:
- Dysfunctional keratinization: The prevailing idea for decades now is that a mysterious combination of factors (including genetic mutations and nutrient deficiencies) cause the cells lining hair follicle (aka the epithelium) to produce too much keratin, resulting in a blockage and subsequent protein buildup.
- Hair shaft malformation: Recent research points to circular patterns of hair growth within the follicle leading to an inflammatory response that includes excess keratin production.
While studies continue, this new hypothesis suggests that the keratin buildup is the skin’s response to abnormal hair growth — that perhaps the problem starts with the hair, not with the skin cells.
What does keratosis pilaris look like?
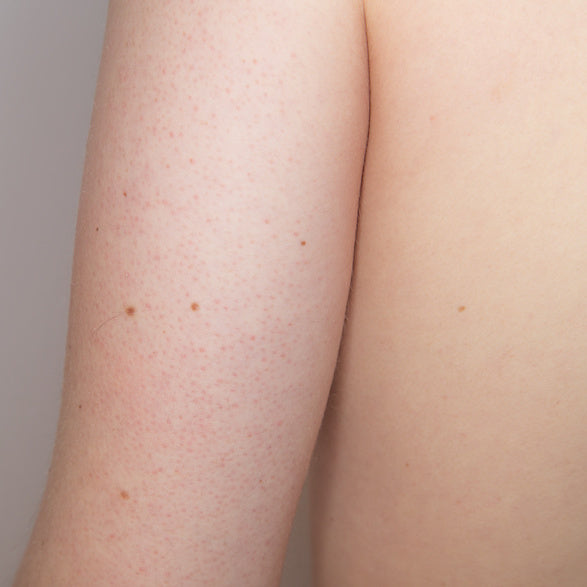
Most often, KP presents as small, hard bumps on the skin’s surface. The bumps can look almost like tiny pimples and feel rough or dry — they may also be itchy and uncomfortable. These bumps tend to be lighter or redder on fair skin and darker on more pigmented skin, but can appear to be white, red, pink, light purple, brown, or black depending on the person’s skin tone.
Keratosis pilaris got the nicknames chicken bumps and chicken skin because the affected area can look like the plucked skin of a chicken. Recently, it's been dubbed strawberry skin for its resemblance to the tiny, rough seeds on the outside of the berry.
Most commonly, KP appears in these regions:
- Upper arms
- Thighs
- Buttocks
- Back
- Cheeks
Keratosis pilaris bumps can appear as just a few spots, or it can overtake an entire area, looking almost like a rash.
Dr. Pimple Popper's KP Picks
Are there different types of strawberry skin?
Yes, keratosis pilaris has a few variants, based on how the condition presents and where on the body it’s found. But the two main types include:
- Keratosis pilaris: Yes, the main condition is simply called keratosis pilaris. It may range from relatively asymptomatic (meaning it shows no sign of illness) flesh-colored bumps, to red, irritated and itchy bumps.
- Keratosis pilaris rubra: This the most common variant of KP, and it’s typically found on adolescent boys. KPR has those signature rough, goosebump-like patches that we’ve been describing, but the skin that surrounds the bumps is bright red.
Who’s more likely to get keratosis pilaris?
As we mentioned above, KP is generally believed to be a genetic condition, as it runs in families. But there’s also a host of things that make it more likely you’ll experience keratosis pilaris, including:
- Age: It’s more common in kids and adolescents.
- Skin concerns: If you’ve got eczema, super dry skin, or a condition like ichthyosis vulgaris, your body is more likely to have that buildup of keratin.
- Allergies/autoimmunity: People who have conditions like asthma or hay fever are more susceptible.
- Obesity: studies have shown a correlation between keratosis pilaris and individuals with a high BMI.
How do you treat keratosis pilaris?
KP isn’t harmful or serious, but it can be a source of frustration if you’re trying to treat it. Although there’s no known cure, there are some options that can help manage the symptoms and improve the bumpy appearance.
According to Dr. Sandra Lee (aka Dr. Pimple Popper), a combination of exfoliants (like alpha hydroxy acids) and moisturizing ingredients is the best way to approach keratosis pilaris. Exfoliating ingredients help slough off the rough keratin buildup, while moisturizers soothe and protect the skin barrier. Her recommendations include these SLMD Skincare products:
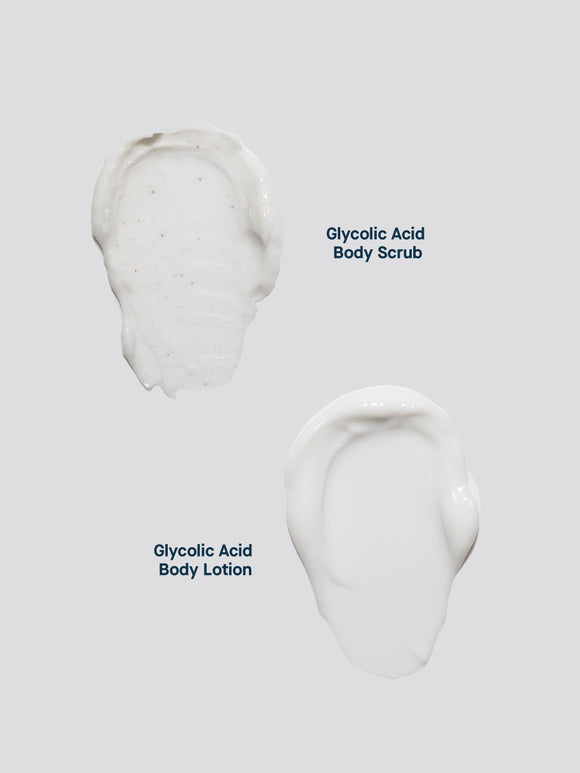
- Glycolic Acid Body Scrub: a physical and chemical exfoliating scrub containing glycolic acid, finely ground volcanic ash, and a deeply-penetrating form of hyaluronic acid.
- Glycolic Acid Body Lotion: an exfoliating moisturizer formulated with glycolic acid, aloe and niacinamide to soothe and soften skin.
These two are available for a special value in the SLMD Body Smoothing System.
If you don’t see the results you’re looking for, consult with your dermatologist about other treatment options, like microdermabrasion or laser therapy.

Dr. Lee's Last Word
Keratosis pilaris is one of the most common skin concerns that I see in my practice. It’s certainly not serious, but it can really affect a person’s quality of life. Fortunately, KP is one of those conditions that typically responds very well to over-the-counter glycolic acid treatment. Most people can manage their KP by using an exfoliating scrub and moisturizer.