Psoriasis is a chronic inflammatory disorder that results in plaque formation on the surface of the skin. The exact cause of this disorder is unknown, but it’s likely the result of problems with the body’s autoimmune system. Psoriasis typically affects the skin on the scalp, joints, hands, and lower body, including the knees, elbows, lower back, feet and genitals.
Adults and children can be diagnosed with psoriasis, but the disorder commonly presents when people are in their 20s. The thick patches of skin associated with psoriasis wax and wane depending on stress levels, environmental conditions and the presence of infection.
Most people who have psoriasis initially assume they have a skin infection or are experiencing an allergic reaction. Once they see a doctor, however, diagnosing psoriasis is relatively easy, but in some cases a skin biopsy is required.
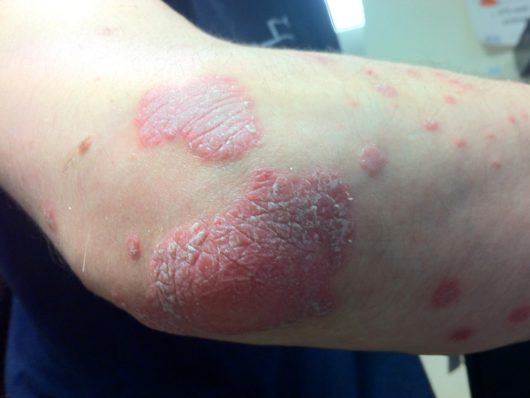
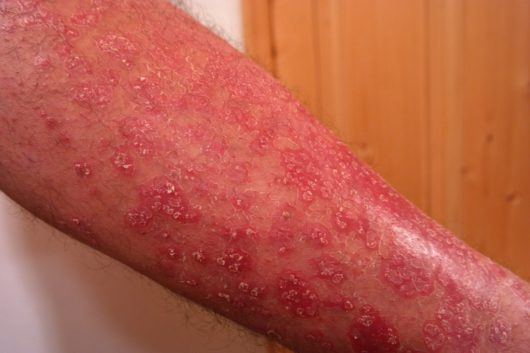
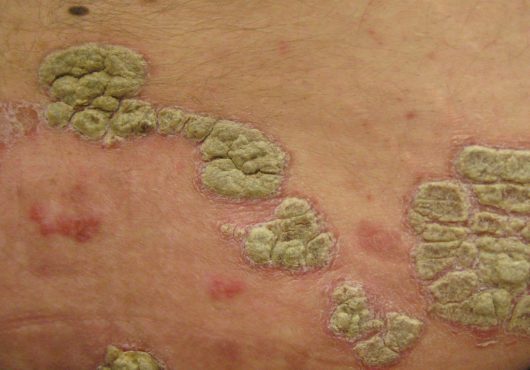
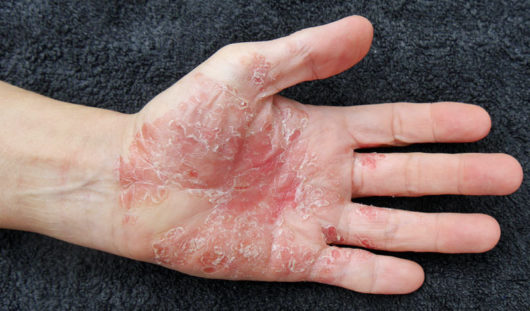
What does psoriasis look like?
This skin disease is characterized by raised, red and silvery irritated patches of dead skin cells that appear on the body’s surface. Those with psoriasis have cells that multiply up to 10 times faster than normal cells. Therefore, psoriasis lesions are produced as a result of this abnormally fast cell production, which causes an excess of cells to build up on the surface. These thick, irritating patches are almost always painful and itchy, and may bleed and crack.
Treating psoriasis
Once psoriasis has been diagnosed, treatment is required. The type of treatment a doctor will advise will depend on how much of the skin’s surface is affected, the thickness of the plaques, and if the individual is also suffering from arthritis. The basic management of psoriasis involves use of topical and systemic medications. Other treatment approaches, which can be used at the same time, include use of phototherapy, moisturizers, salicylic acid, and urea. Stress reduction is also a vital part of treatment, as doctors believe stress levels are a major factor in psoriasis flare ups.
Over the years many guidelines have been developed for the treatment of psoriasis. When topical medications fail to work, most people are treated with systemic medications. Methotrexate is the drug that’s often prescribed; for more severe cases, doctors may suggest cyclosporine. While these drugs may work well to treat the condition, they aren’t entirely effective.
Is there any new research on, or new treatments for, psoriasis?
For much of the past 30 years, the treatment of psoriasis had remained stagnant and many patients experienced poor quality of life, mainly because prescription drugs don’t work reliably. There are also a significant number of patients who are unable to tolerate these therapies — or develop intolerable side effects.
In the last decade, several new agents have been developed to treat psoriasis. Because researchers and doctors have a better understanding of the role of that the immune system plays in psoriasis, they have been able to develop a newer class of drugs, known as targeted biological agents. There is good evidence indicating that these biological agents are very effective in treating psoriasis. This breakthrough has led to a new era in the management of this complex disorder.
These biological agents are proteins or antibodies that have been manufactured in a lab. Once injected itno the skin, they block or alter the immune system that is known to contribute to psoriasis. This helps limit both inflammation and damage to the joints. By interfering with specific immune cells (T cells), these biological agents simultaneously reduce the overgrowth of thick scaly skin that makes psoriasis such a recognizable, and difficult, disease.
The biological agents currently approved for the use of moderate to severe psoriasis are:
– Adalimumab (Humira)
– Etanercept (Enbrel)
– Infliximab (Remicade)
– Secukinumab (Cosentyx)
– Ustekinumab (Stelara)
Evidence from clinical trials suggests that these agents can reduce the symptoms and signs of psoriasis in more than 75% of patients. But, like most medications, these newer agents have several negatives: They have to be injected; are incredibly expensive; require close monitoring, as they can increase the risk of infections like tuberculosis; may be associated with higher risk of cancer; and sometimes cause allergic reactions.
Scientists are continuing to learn more about the cause of psoriasis so that better, more effective therapies can be developed. Recent genetic work indicates that within a few years, there will be a genetic test to help screen individuals who are at risk for psoriasis. There is hope that more specific drugs targeting precise components of the immune system will not only lead to more effective psoriasis therapy and have fewer side effects.





It’s so great to finally hear a famous doc talking about this.
I’m Brazilian and I have arthritis psoriasis. I take remicade every 8 weeks, but before I find out I’ve been through so much pain.
I admire a lot of your work Dr. Pimple and I feel very happy for you to talk about different kinds of diseases.
Can psoriasis be mistaken as eczema? I have had a patch on my leg for over a year now and have been using a topical cream (Betamethasone Dipropionate?) for treatment. It has helped, but this patch isn’t going anywhere. It is thick, dry and flaky. Before I started the cream, it would leak a watery fluid when scratched. My doctor said to continue the cream twice daily for three months until I see her again. It hasn’t spread, nor have I experienced anything similar, in my short 22 years. No family members suffer from eczema or psoriasis. Any guesses?
I have psoriasis gutatta and have been on methrotexate, chemo-phototherapy, and trued many if not all topical steroids. The only thing that has “cured me” has been my pregnancy. Absolutely ALL signs of paoriasis disappeared, even though my stress levels from a high risk pregnancy were very high.
My dermatologist suggests trying different methods every two years. Ive done chemophototherapy before I got pregnant, steroids, and retinoids. Biologicals seem like the next step. I see that you say chances of cancer increase with it… how ever so does chemo-phototherapy. What should i do? Planning on another baby in the next year…
I have guttate psoriasis, too. Sounds like yours, unfortunately is worse than mine. I also love the pregnancy bit, too. It’s all about the immune system when your pregnant.
Mine goes away for a few years after. Mine is rather mild, although my current outbreak is a first of its kind for me! I’m spotted all over except my face and neck. My trunk and legs had spots all over.
I assume they did a strep test for you? They did for me and yes, I had the strep virus in my system, which triggers guttate type. 2 rounds of antibiotics and creams and a shot. Nothing will help if you have that in your system. I remember years ago having to be on antibiotics for months…
Best of luck, my guttate/gutatta friend.
I hate to sound glib, but it sounds like you need to stay pregnant. I have plaque psoriasis on my scalp and in my ears. My stress levels stay high as I am a caregiver to my mom, who has dementia. Sadly, I have infertility issues so pregnancy isn’t an option for me.
Same story for me… Good luck dear !
I’m lucky-when I have flare ups they’re not bad. The only ones I can’t seem to clear up are the ones on my scalp. The clobetasol solution runs off, and I have a hard time getting the ointment where it needs to go because of my hair. Is there anything else I can do to get these areas cleared up?
What do you do when all above approaches fail to work? Is there anything that can provide itchy relief while the plaque takes over?
Psoriasis is an ailment no one likes to deal with. There are no cures but there are ways to prevent outbreaks and deal with symptoms. There are many medications and creams that can be used to treat psoriasis, but they require constant use and can cost lots of money over time. The best thing to do for yourself is to change your lifestyle and prevent the outbreaks.
Some lifestyle changes are simple, while others are more difficult. Finding ways to prevent psoriasis outbreaks is a search any sufferer is willing to pursue. The first way to change your lifestyle is to change your diet. Changing your diet can help you lose weight, which may be a factor in triggering psoriasis. Add more fruits and vegetables to the diet and try to remove salts and fats. Use sugars in moderation and watch that cholesterol.
Smoking can trigger outbreaks, so changing your lifestyle towards smoking cessation is a great idea. There are many ways to stop smoking from chewing gums to patches and pills. The sooner you can stop this habit the better. Smoking increases your chances of developing psoriasis in the first place. If you already have psoriasis, your chance of frequent flare-ups is greater if you are a smoker.
Drinking alcoholic beverages also increases your changes of outbreaks. Heavy drinking can bring on psoriasis as well. Doctor’s will advise patient’s to limit the amount of alcohol they drink because alcohol seems to be linked to flare-ups. If you are currently experiencing an outbreak, it is a good idea to lay off the alcohol until it subsides. Heavy drinking will also cause frequent flare-ups and prevent the disorder from ever fully going away.
The final lifestyle change is a focus on stress reduction. Stress is a huge trigger of psoriasis, probably one of the biggest. Learning ways to manage stress is important for anyone who suffers from the disease. Take some time out of the day to relax, enjoy a book, or take a brisk walk. Try not to take on too much at work and ask for help if needed. Reducing the amount of stress in your life will help prevent future flare-ups.
Psoriasis being an autoimmune condition can be treated via diet. The GAPS diet has been effective in controlling and eliminating this condition. Because it is not a drug that the pharmaceutical industry can make money from, further research and information on it have not been conducted
I’ve been worried that my daughter might have the beginning of psoriasis as she’s had a small area of red start to form. I liked that you had mentioned that once it’s diagnosed treatment is required and a doctor will be able to explain how to fully treat it. If the area starts to get worse, I hope I can find a doctor that can figure out the best method to use to diagnose and treat it.
My mom Has a severe cases of this on her foot, sometimes it is so painful she can barely walk, she use a certain type of injection, enbrel, my question is can this affect her Breathing? She recently was hospitalized for her breathing issue and now she’s on oxygen daily at home, can these 2 things be related
Thanks for the info. My brother has this on his skin. We are now looking up some health professionals to help him with it.
I started taking CBD oil to help me get off of morphine i had taken for 16 years. It works well for pain and it came with an added bonus. It cleared up the psoriasis on my hands! First time in over 20+ years. I have tried everything my Dr’s could think of over the years and nothing made it go completely away like this. I still have a small patch on the back of my neck but I’m hopeful it will go away forever and l’ll be CURED by CBD Oil…….I’m done with big pharma!…oh and I’m also losing 1-2 pounds a week!!! and I’m not even trying.
What kind of oil did you use? I keep seeing oil and tincture and I’m not sure the difference. Also, if you ordered online do you mind sharing the website. Thanks!
What about Otezla (pill)? I started this in December and have seen improvements already.
I have scalp psoriasis and its been since 4years i have it
Now i am having a homeopathic treatment but would like to know if theres a quick soution to it please help
i can’t even make friends like before
I’ve been dealing with this disease for a long time now. I empathize with everyone coping with psoriasis as I know it’s been very hard for me as well. As most of you, I’ve been to a lot of doctors and I’ve been prescribed a bunch of treatments. Some worked for a while, but never really “cured” me some even gave me some severe side effects. I know there is no cure unfortunately. At this time I’m trying a cream that is custom made with natural ingredients like: rapeseed oil, candelilla wax and shea butter. It’s too early to give you a certain answer if this helps or not, but I’m going to use it and I’ll come back in a couple months and update you with my progress. Stay strong!
My boyfriend has guttate psoriasis that developed in his early twenties. He tried medication for a while, granted there are probably better things out there now. The side effects were worse but it did get his intital flame up down. He now treats his psoriasis by keeping his skin overly moisturized, going to the tanning bed, and swimming or soaking in salt water whenever possible. The tanning bed or being out in the sun really helps when he is having a large flare up to get it back in control! Just staying connected with his doctor to constantly check for signs of skin cancers!
I have had plaque psoriasis since I was 12 and I’ll be 50 this year. I have tried many different treatments, but honestly was has worked best is tanning bed. I know they say it’s bad but with the side effects and greasy stuff and whatever else. I can say I has very little as of now if I only go 1 it 2 times a week it’s keeps it where it’s manageable
Thanks for the great information on recognizing and treating psoriasis. I had no idea that a combination of topical and systemic medications are used to treat psoriasis and that they can contain salicylic acid and urea. It sounds like it would be very useful to visit a dermatologist and begin a treatment plan for your skin.